A Closer Look at Oncology Imaging

Nishant Verma, MD
QUESTION: What is SMIL’s process for imaging NETs?
ANSWER: Neuroendocrine tumors (NETs) are rare malignancies that are increasing in incidence. Surveillance, Epidemiology, and End Results (SEER) data shows the age-adjusted incidence of NETs rose from 1.9 to 5.25 cases per 100,000 people between 1973 and 2004. Nearly a third of neuroendocrine tumors develop within the small bowel (SBNETs).
These SBNETs, also called carcinoids, are often small and lack symptoms until metastases develop. Surgery is the only cure in localized disease and may also play a role in advanced disease. As a result, preoperative imaging is important for staging, localization of unknown primaries and treatment planning.
The two most common imaging modalities are CT scan and octreotide scan, or somatostatin receptor scintigraphy (SRS). In a retrospective comparison of patients with SBNETs at the University of Iowa, researchers found that SRS found four primary tumors missed by CT, while CT identified five tumors missed by SRS. They concluded that the two modalities are complementary.
In the situation of inconclusive CT scan, an octreotide scan can resolve the question of malignancy. Nuclear Medicine Specialist Nishant Verma, MD, of Scottsdale Medical Imaging (SMIL), says the problem with SRS is that the resolution is very low.
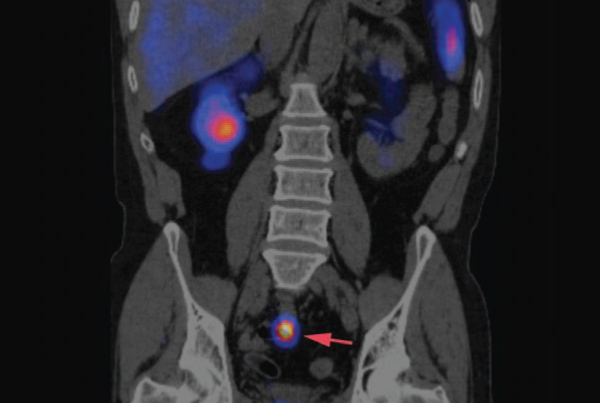
“We can often see tumors but may have difficulty localizing them,” Verma says. “To overcome that, we use SPECT-CT (single-photon emission computed tomography) to make a 3-D reconstruction of the octreotide data, and fuse it over the CT data. This allows us to look at both studies simultaneously and correlate the abnormality on the octreotide scan with the mass on the CT. It really adds a huge advantage in our ability to detect these lesions.”
SMIL is one of few radiology groups using SPECT-CT for NETs, Verma says. He recommends that it be the first step in investigating suspected endocrine tumors, in part because they can also treat the tumor using the octreotide receptors.
“Knowing a tumor is positive on our scan, we administer a similar molecule that binds to the somatostatin receptor and basically shuts the cell down. In this way, the imaging not only identifies the disease but can guide treatment as well.” •
REFERENCES:
Yao JC, et al. One hundred years after “carcinoid”: Epidemiology of and prognostic factors for
neuroendocrine tumors in 35,825 cases in the United States. J Clin Oncol. 2008;26(18):3063-72.
Dahdaleh F, et al. The value of preoperative imaging in small bowel neuroendocrine tumors. Ann
Surg Oncol. 2013;20:1912–1917.

